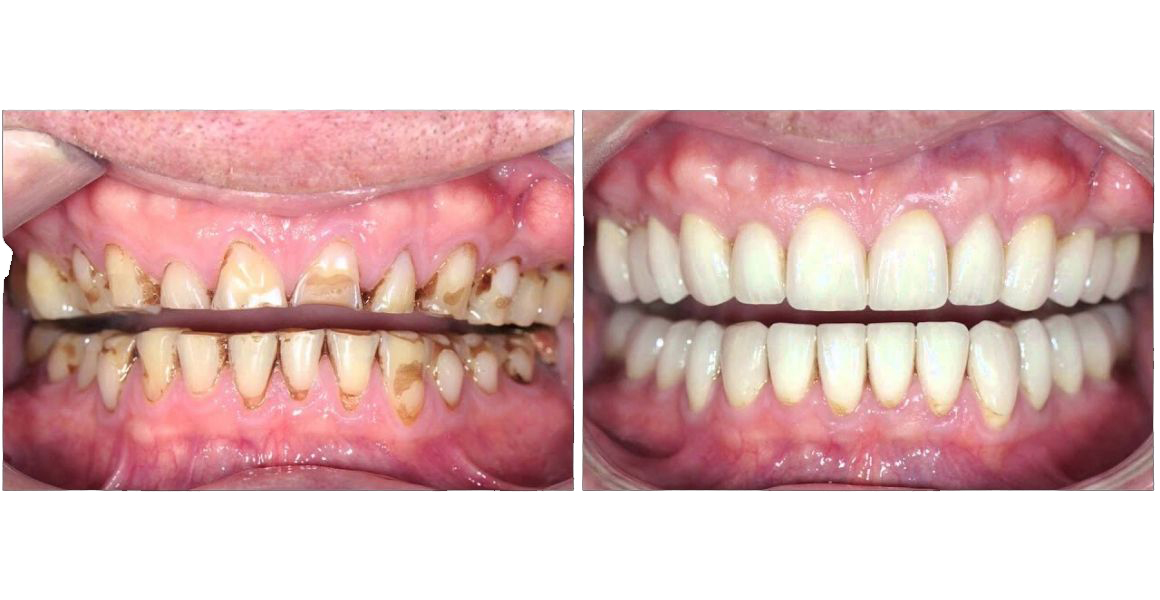
Full Mouth Rehabilitation
Full mouth rehabilitation or full mouth restorations is a term used to describe the process of simultaneously rebuilding or restoring all or most of the teeth in your mouth.
Full mouth rehabilitation typically involves our team of general dentists and restorative dentist who will perform procedures like teeth capping bridging or veneers.
It may also involve a gum specialist (Periodontist) to cut your gums to make your teeth longer, and oral surgeon, an orthodontist act ( to move your teeth in the right position) and an endodontist (Root Canal Specialist).
So usually full mouth rehabilitation is teamwork performed by the specialist of each field at world Smiles Dental Centre.
The need for full mouth rehabilitation may result from an
- Teeth completely lost Due to decay or trauma
- Broken down or fractured teeth
- Teeth that have severely worn out due to faulty biting pattern for tooth grinding.
- An ongoing complaint of jaw and muscle pain or headache requiring bite correction
The diagnosis for a Full Mouth Rehabilitation Case
- The 1st step in treating a patient who requires full mouth rehabilitation (FMR) is coming to the right diagnosis.
- Most patients come with referred pain in the joints around the ear or around the temple. There is also some pain or soreness in the muscles around the cheek and joints.
- The mouth opening may be restricted or reduced too in some cases. All these sometimes leads to confusion in the patient’s mind as to what and where does the problem underlie.
- At World Smiles dental center, Dr Rohan Bandi who is a specialist in treating innumerable patients with similar problems will help you understand the cause of your problem.
- Detailed examination of your jaw muscles, joints and teeth is done.
A diagnostic device called an Anterior Deprogrammer is given to you to wear for a couple of days. (FIG: 1)


Most patients find immediate relief in symptoms and report of the comfort they felt in the night while sleeping and when waking up in the morning.
This step confirms our diagnosis and usually is the building block and basis for us to proceed to the next stage which is recording your jaw movements and studying them on a jaw simulator called a Semi-adjustable articulator. (FIG: 2)


The jaw movements and how these movements affect your teeth causing the damage are shown to you live.
After this explanation and understanding, a decision and call is taken as to what is the best way to treat the problem.
Whether full mouth caps and bridges are required or only some teeth are required to be capped and rest can be shaped into the right biting position.
All these are discussed with the patient before finalizing the treatment plan.
Once a consensus is reached only then treatment is started.
In such cases diagnosis, and finding and correcting the cause of the damage is more important than the treatment itself. Most doctors and practitioners neglect or are unaware of this critical and most important step/part.
The Treatment
The treatment involves shaping the teeth for caps or modifying them to the right shape.
After which temporary caps are given.
You are on temporary caps for a while, until your symptoms and pain is gone and you are comfortable with your new teeth and biting.
Once you give a go ahead and we are satisfied, the temporary caps are replaced with permanent ones which are beautifully handcrafted or computer generated to exactly fit and suit your mouth. The entire process can take a few weeks to complete.
Since the permanent caps are just a replica of your temporary teeth, you are just as comfortable and pain-free as before.
Your quality of life and health also improves as you are no longer suffering in the morning or night with soreness in the head or jaw joints and muscles.
Your smile is rejuvenated just like you had in your younger days or even better, giving you a big confidence boost. (FIG: 3)